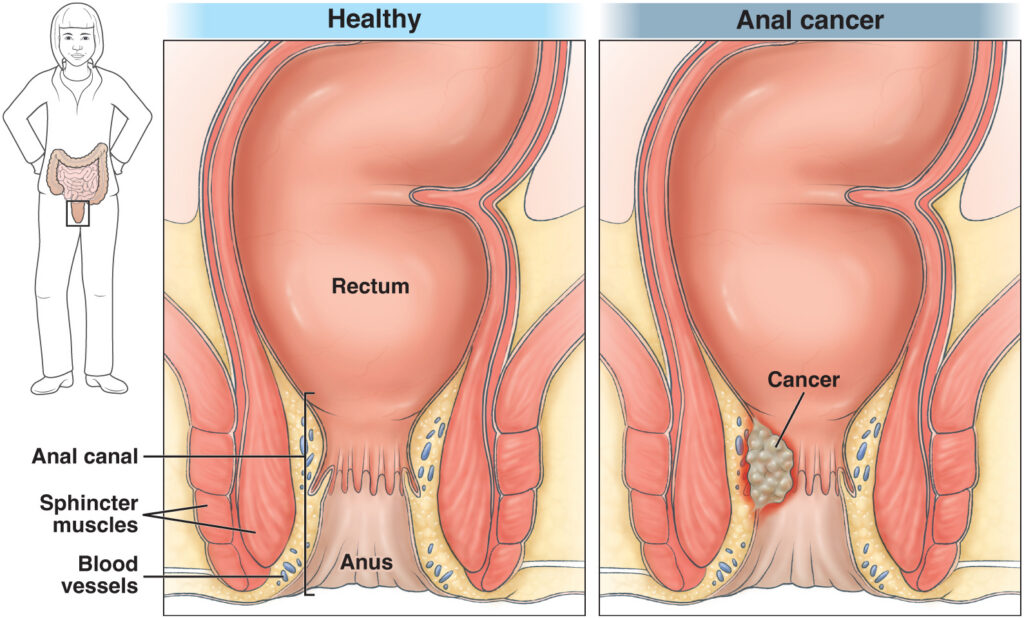
What is anal cancer?
Anal cancer is a type of cancer that develops in the tissues of the anus — the opening at the end of the digestive tract. While it is not common in the general population, the number of cases has been rising steadily over the past several decades. The good news: anal cancer is often preventable and highly treatable when caught early.
More than 90% of anal cancers are caused by human papillomavirus (HPV), a very common sexually transmitted infection. Just like HPV can cause cervical cancer, it can also cause changes in the cells of the anus that may eventually become cancer if left untreated.
Who is at higher risk of anal cancer?
Certain groups of people have a higher chance of developing anal cancer. You may be at increased risk if you:
- Are living with HIV.
- Are a man who has sex with men (MSM).
- Are a transgender woman.
- Have received an organ transplant (and take immunosuppressive medications).
- Have a history of cervical, vulvar, or vaginal cancer or precancer.
- Have a history of genital or anal warts.
- Smoke cigarettes.
- Have an autoimmune condition requiring immunosuppressive therapy.
- Have inflammatory bowel disease (especially perianal Crohn’s disease).
Having one or more of these risk factors does not mean you will get anal cancer — it means you should talk to your health care provider about whether screening is right for you.
What are the symptoms of anal cancer?
Anal cancer often has no symptoms in its early stages. When symptoms do appear, they can be easy to mistake for common, harmless conditions like hemorrhoids. That is why screening is so important for people at higher risk.
Symptoms to watch for include:
- Bleeding from the anus or rectum (blood on toilet paper or in the stool).
- Pain, pressure, or discomfort in the anal area.
- Itching around or inside the anus.
- A lump or mass near the anus.
- Changes in bowel habits.
- Unusual discharge from the anus.
- Swollen lymph nodes in the groin area.
Important: Do not assume that bleeding or pain is "just hemorrhoids." If you have any of these symptoms — especially if they don’t go away — tell your health care provider and ask to be evaluated.
Screening for anal cancer
There are several ways to screen for anal cancer and the precancerous changes, called high-grade squamous intraepithelial lesions, or HSIL, that happen before anal cancer.
Your health care provider inserts a gloved, lubricated finger into the anus to feel for lumps, masses, or other abnormalities. This is a simple, quick exam that can be done in a regular office visit.
Similar to a cervical Pap smear, a small swab is used to collect cells from inside the anal canal. These cells are examined under a microscope for abnormal changes. This test is painless and takes only a few seconds.
A swab is used to test for high-risk strains of HPV (the virus that causes most anal cancers). This may be done alone or together with an anal Pap test (called “co-testing”).
If your screening tests are not normal, you may need this specialized procedure. Your health care provider will use a magnifying instrument (similar to a colposcope used for cervical exams) along with special dyes to closely examine the anal canal and identify precancerous areas. Small tissue samples (biopsies) can be taken during this procedure. HRA requires specialized training and is not available everywhere.
Who should be screened for anal cancer and when?
Recent guidelines from major medical organizations recommend the following:
If you are living with HIV:
- Men who have sex with men and transgender women: Begin screening at age 35
- All other people with HIV: Begin screening at age 45
Annual assessment of anal symptoms and a digital anorectal exam is recommended for all people with HIV, regardless of age
If you are NOT living with HIV:
- Men who have sex with men and transgender women: Consider screening starting at age 45
- Solid organ transplant recipients: Consider screening starting 10 years after transplant
- People with a history of vulvar precancer or cancer: Screening within 1 year of diagnosis
- People age 45 and older with a history of cervical or vaginal precancer/cancer, perianal warts, or autoimmune conditions: Discuss screening with your health care provider
Your health care provider can help you decide the best screening plan based on your individual risk factors.
What happens if screening finds something abnormal?
If the results of your anal pap test or HPV test are not normal, your health care provider will likely refer you for high-resolution anoscopy (HRA). During HRA, if precancerous areas (HSIL) are found and confirmed by biopsy, they can be treated. Treatment options include:
- Electrocautery (burning off the abnormal tissue — the most commonly used method).
- Topical medications (such as fluorouracil or imiquimod cream).
- Surgical removal.
A landmark clinical research trial called the ANCHOR study showed that treating these precancerous lesions reduced the risk of developing anal cancer by 57% in people living with HIV. This is why finding and treating precancer matters.
If the results of your anal pap test or HPV test are not normal, your health care provider will likely refer you for high-resolution anoscopy (HRA). During HRA, if precancerous areas (HSIL) are found and confirmed by biopsy, they can be treated. Treatment options include:
- Electrocautery (burning off the abnormal tissue — the most commonly used method).
- Topical medications (such as fluorouracil or imiquimod cream).
- Surgical removal.
A landmark clinical research trial called the ANCHOR study showed that treating these precancerous lesions reduced the risk of developing anal cancer by 57% in people living with HIV. This is why finding and treating precancer matters.
How can you prevent anal cancer?
How to advocate for yourself
Anal cancer screening is still not as widely known or routinely offered as other cancer screenings. Here is how you can take charge of your health.
-
Know your risk factors
Review the list above. If any apply to you, bring it up with your health care provider — even if they don't ask.
-
Ask directly
You can say: "I understand I may be at higher risk for anal cancer. Can we talk about whether I should be screened?" or "I'd like to have an anal Pap test — is that something you can do or refer me for?"
-
Don't be embarrased
Anal health is a normal part of medical care. Health care providers are trained to discuss these topics, and your health is more important than any awkwardness.
-
Request a digital anorectal exam
This is a simple exam that any primary care provider can perform. If you are in a higher-risk group, it should be part of your routine care.
-
Ask about HRA access
If your screening results are not normal, ask your health care provider to refer you to a specialist who performs high-resolution anoscopy. Not all providers offer this, so you may need to seek out a specialized center.
-
Keep records
Track your screening results and follow-up appointments. If you have had abnormal results in the past, make sure your new providers know.
-
Seek a second opinion if needed
If your concerns are dismissed, you have every right to seek care from another provider. Organizations like the International Anal Neoplasia Society (IANS) maintain resources to help patients find screening providers.
-
Know that disparities exist
Screening availability varies by region, and certain communities face greater barriers to care. If you are having trouble accessing screening, ask about telehealth options, community health centers, or clinical research trials that may offer screening.
Key takeaways
1. Anal cancer is caused by HPV and is largely preventable.
2. People at higher risk — especially those living with HIV, men who have sex with men, transgender women, organ transplant recipients, and people with a history of HPV-related cancers — should talk to their health care providers about screening.
3. Screening is simple and can include a digital exam, an anal Pap test, and/or HPV testing.
4. Treating precancerous changes can significantly reduce your risk of developing anal You are your own best advocate. Don't hesitate to ask your health care provider about anal cancer screening.
Resources and communities
- The Anal Cancer Foundation is dedicated to empowering patients with anal cancer and accelerating prevention and research methods that eliminate anal cancer and the virus that causes the majority of cases, HPV.
- The Farrah Fawcett Foundation honors Farrah Fawcett’s Fight with cancer by giving to: cutting-edge HPV-related cancer research in memory of Farrah’s life and fight to the end; patient assistance funds for those faced with mounting expenses during treatment; and prevention programs to help spread the word so the cancer struggle will cease.
- HPV Cancers Alliance is a national nonprofit committed to reducing the burden of HPV through comprehensive education, prevention, and advocacy by providing trusted, evidence-based information on HPV infection, vaccination, and cancer prevention—alongside emerging research and updates on HPV-related cancer treatment.
- The International Anal Neoplasia Society is the world’s first professional society devoted to the prevention and treatment of anal intraepithelial neoplasia and anal cancer.
Written by

Jessica D. Korman, MD
Capital Digestive Care, Washington, DC
AGA Patient Education Advisor
April 2026